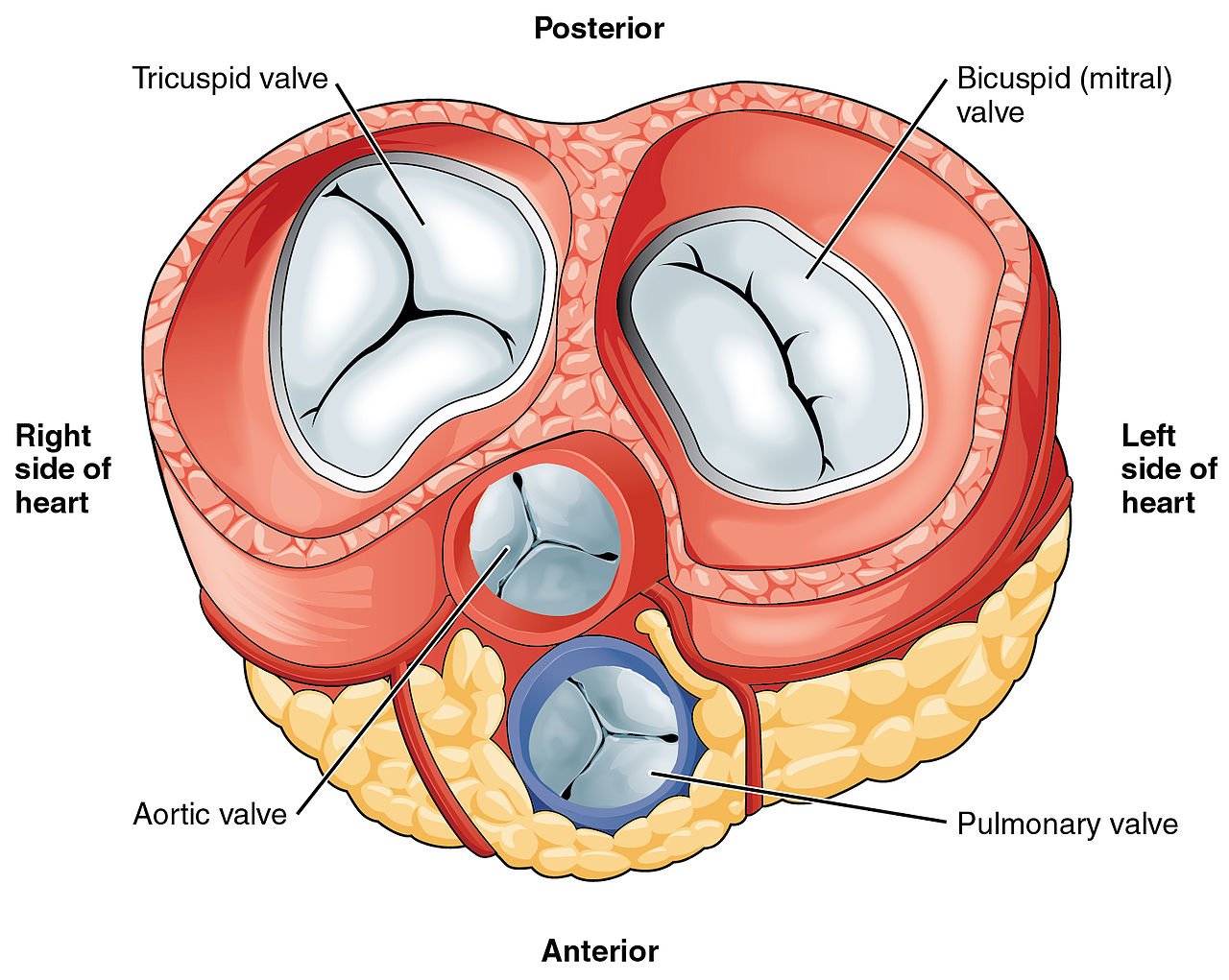
Singapore – Bicuspid aortic valve (BAV) is the most common congenital heart defect in which patients are born with two flaps in their aortic heart valve instead of the usual three. However, there isn't a personalized approach for preventing the complications resulting from this defect.
Supported by a $3.3 million National Institutes of Health (NIH) RO1 grant, Dr. Paul Fedak, cardiac surgeon and professor in the departments of Cardiac Sciences and Surgery and Alex Barker, PhD, Northwestern University Feinberg School of Medicine will use 4D-Flow MRI, a cutting-edge imaging technique that allows visualization of three-dimensional blood flow in real time, and tissue analysis to inform personalized treatment for BAV patients. The results of the study may cut down on the number of unnecessary open-heart surgeries while also identifying and targeting those who are at highest risk and need it most.
"Not all BAV patients are the same, yet they are currently treated the same when it comes to timing and extent of surgery," said Fedak. He added, "Through this study we can give clinicians and surgeons the tools they need to create precise, individualized treatment plans for patients."
"Each patient's condition is unique. We are developing state of the art MRI techniques to help with the assessment of their condition to develop the best plan of treatment," said Barker, a bioengineer and assistant professor in the Department of Radiology at the Feinberg School of Medicine.
BAV affects more than seven million people in North America, and 50 percent of them will require a life-saving intervention such as open-heart surgery.
The NIH grant will allow for advanced tissue analysis for a large group of patients (450) over the next five years, the largest series in the world. Recruitment is already underway.